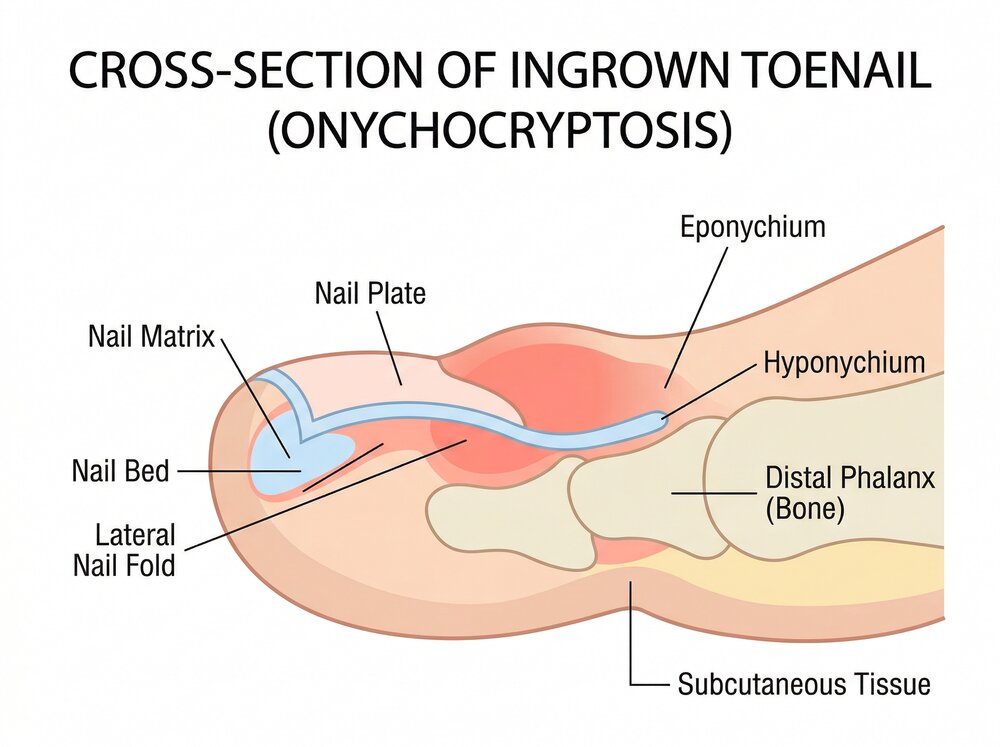
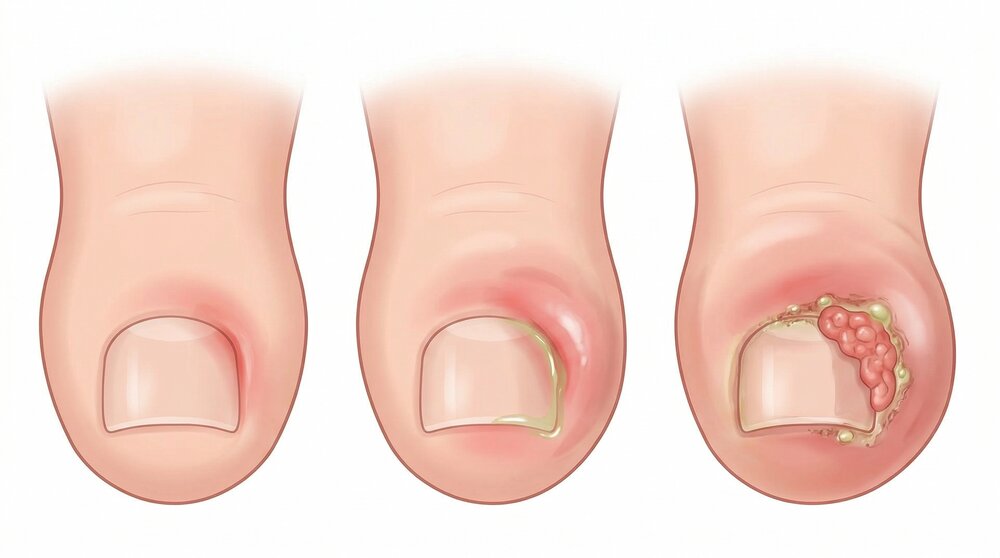
What Is an Ingrown Toenail?
An ingrown toenail (onychocryptosis) occurs when the edge of a toenail grows into the surrounding skin, causing pain, swelling, redness, and sometimes infection. The big toe is most commonly affected, though it can occur on any toe.
Ingrown toenails are one of the most common foot problems in Australia, affecting an estimated 2.5–5% of the population. They account for approximately 20% of all foot-related presentations in primary care.
While mild cases may respond to conservative care, moderate to severe ingrown toenails often require a minor surgical procedure called a wedge resection to provide lasting relief.